When there is an abnormally high force required to pump blood through the blood arteries, a condition known as high blood pressure or hypertension develops. Many people with hypertension don’t experience any noticeable symptoms until they get their blood pressure checked. Uncontrolled high blood pressure increases the risk of stroke, heart disease, and other cardiovascular complications. Fortunately, the risks associated with hypertension can be mitigated by the use of medication and adjustments in lifestyle.
- Why Do I Sleep So Much? Comprehensive Guide Update 04/2026
- The Relationship Between Sleep and Mental Health Update 04/2026
- How To Make Mattress Firmer? Finding the Right Mattress Firmness Update 04/2026
- Coronasomnia: Symptoms, Risk, Causes and 6 Solutions for Better Sleep Update 04/2026
- How Can Noise Affect Your Sleep Satisfaction? 3 Tips to Get Better Sleep Update 04/2026
The sleep disorder known as sleep apnea is characterized by periodic stops in breathing while sleeping. The two forms of sleep apnea are obstructive sleep apnea (OSA) and central sleep apnea (CSA). Periods of airway collapse characterize OSA, preventing air from reaching the lungs and leading to snoring and gasping during sleeping. A breakdown in neural connectivity between the brain and the respiratory muscles underlies the episodic cessation of breathing seen in CSA.
Bạn đang xem: How Sleep Apnea Affects Blood Pressure? A Perfect Guide For You! Update 04/2026
When a person has both hypertension and sleep apnea, treating the latter can help reduce the former’s effects on blood pressure.
What is Hypertension?
Blood pressure is the result of the force of blood pushing against the artery walls; hypertension develops when this force is too great. As a result, your heart muscle becomes overworked and exhausted, preventing it from performing at its best.
Hypertension comes in a wide variety of forms, some of which are:
- Lung or Arterial Hypertension (PAH).
- An Unresponsive Hypertension.
- An increase in blood pressure throughout the body.
- High blood pressure that does not respond to medication.
You’ve probably had your blood pressure checked before at the doctor’s office and experienced the uncomfortable squeeze on your arm while the machine recorded your reading. Your systolic blood pressure is the higher figure and your diastolic blood pressure is the lower number that you’ll find in your results.
- The amount of force your blood pumps through your arteries at each heartbeat is represented by your systolic blood pressure.
- The pause in your heartbeats, or diastole, is what determines your diastolic blood pressure.
Although fluctuations in blood pressure during the day are to be expected, continuously high blood pressure is not normal and may suggest hypertension and other issues.
How Hypertension Affects Your Body
Almost half a million people in the United States lose their lives every year due to high blood pressure. The Center for Disease Control and Prevention reports that 32.6-38.6% of Tennesseans aged 20 and up have hypertension.
Xem thêm : Sleep And School Performance: What Is the Effect of Poor Sleep on School Performance? Update 04/2026
When mistreated, hypertension can cause heart failure and other serious health problems, including disability and even death. These include some of the following:
- The Stroke of Heart Disease
- Cardiovascular disorder characterized by irregular heartbeats (atrial fibrillation).
- Aneurysms.
- A heart attack or cardiac arrest.
- Deterioration of the Eyes’ Ability to See.
- Stroke.
- Disease of the kidneys or inability to function properly.
Risk Factors for Hypertension
One of the most prevalent risk factors for hypertension is becoming older, however gender and family history also play a role. Although hypertension is extremely prevalent in the adult population of the United States, there are no outward manifestations of the disease. In light of this, it is sometimes referred to as “the silent killer.”
Diseases of the cardiovascular system, including heart disease, heart failure, stroke, and erectile dysfunction, are all linked to hypertension. Sleep apnea, commonly known as sleep disordered breathing, is associated with many medical issues. Anyone experiencing high blood pressure might benefit from a sleep test, as studies show that up to half of those with hypertension also have sleep apnea.
Hypertension, on the other hand, can be effectively managed with a change in diet, improved sleep hygiene, and regular physical activity. If your hypertension doesn’t improve after trying these measures, including medication, it’s crucial to have a sleep study performed to rule out sleep apnea as a cause.
The Relationship Between Sleep Apnea and Blood Pressure
Only obstructive sleep apnea (OSA) has been associated with an increased risk of hypertension. Despite the fact that CSA is not a known cause of hypertension, it appears in 30-50% of persons with heart failure.
It is believed that 4-7% of the general population suffers from OSA, but that number rises to 30-40% in those with hypertension. It is estimated that almost half of those who have been diagnosed with OSA also have hypertension.
“Blood pressure dipping” describes the normal nighttime drop in blood pressure that occurs in healthy people. This drop can be as much as 20 percent. People with severe OSA have what is known as a “non dipping” blood pressure pattern, which means their blood pressure rarely drops by more than 10%.
Anyone whose blood pressure stays consistently high during the night is at a higher risk of developing cardiovascular problems. Additionally, many people with OSA have hypertension that is particularly severe upon awakening. This “morning rush” could be a contributing element to the development of cardiovascular disease. All-cause and cardiovascular mortality are both raised by moderate to severe OSA.
The impact of OSA on blood pressure extends beyond the overnight hours. The degree of sleep apnea has been shown to correlate with a rise in daytime blood pressure.
How Does Sleep Apnea Cause High Blood Pressure?
Sleep deprivation puts stress on the heart, and obstructive sleep apnea (OSA) in particular triggers an overactivation of the sympathetic nervous system, which may result in hypertension. Our “fight or flight” reaction is regulated by the sympathetic nervous system. When triggered, the sympathetic nervous system causes a transient rise in heart rate, blood pressure, pupil size, and metabolic rate, among other effects. All of these alterations help us respond to stressful situations, but prolonged sympathetic nervous system activity has been linked to hypertension.
Xem thêm : How Long Do Cats Sleep? Cats Sleep Much More Every Day than Humans Update 04/2026
When a person with OSA experiences airway collapse and stops breathing for even a short period of time while sleeping, their sympathetic nervous system is engaged and their blood pressure quickly rises once they start breathing again. This pattern of interrupted and resumed breathing can sometimes startle a sleeping person awake. A person’s sympathetic nervous system is further activated and their blood pressure is higher when they awaken from an OSA episode.
Catecholamines, hormones of the sympathetic nervous system, are also released into the blood when sleep is disrupted by OSA symptoms. The adrenal glands are responsible for releasing the stress chemicals known as catecholamines. Catecholamines contain substances like dopamine and epinephrine (also called adrenaline). High blood pressure is caused by an excess of catecholamines in the body.
Obesity and Insulin Resistance
The interplay between obstructive sleep apnea (OSA), high blood pressure (BP), obesity, and insulin resistance is intricate, with each condition influencing and exacerbating the others.
A higher risk of developing OSA is observed in the obese. As with hypertension, obesity is linked to a higher risk of cardiovascular disease. There is evidence to suggest that a person’s cardiovascular health can be negatively impacted by having both OSA and being overweight. Elevated leptin levels are associated with a number of health issues, including sleep apnea and obesity. One more factor that can lead to weight gain is the hormone leptin. Furthermore, Leptin places strain on the cardiovascular system, which may contribute to the onset of hypertension.
When it comes to using glucose, a kind of sugar in the blood, for energy, people with insulin resistance need increasingly large doses of the hormone insulin. Long-term insulin resistance can cause high blood glucose levels and eventually diabetes. Insulin resistance is commonly associated with obesity. Recent research has demonstrated that OSA contributes to insulin resistance independently of body mass index. However, high blood pressure is an independent risk factor for insulin resistance. High blood pressure may be caused by or made worse by insulin resistance due to the activation of the sympathetic nervous system.
How Does Sleep Apnea Treatment Affect Blood Pressure?
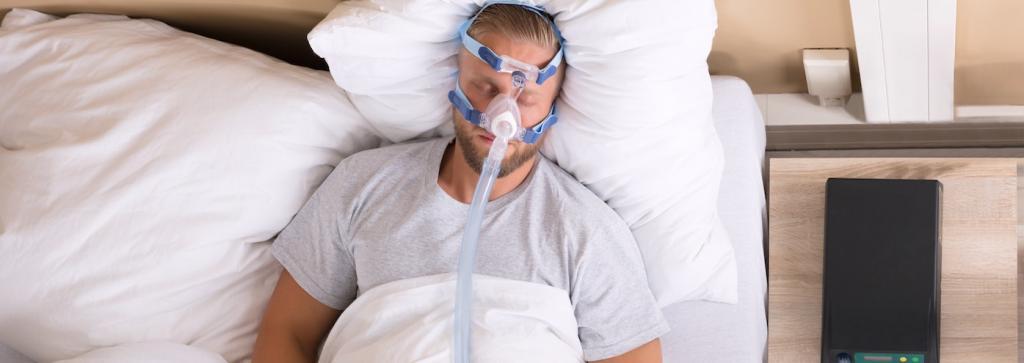
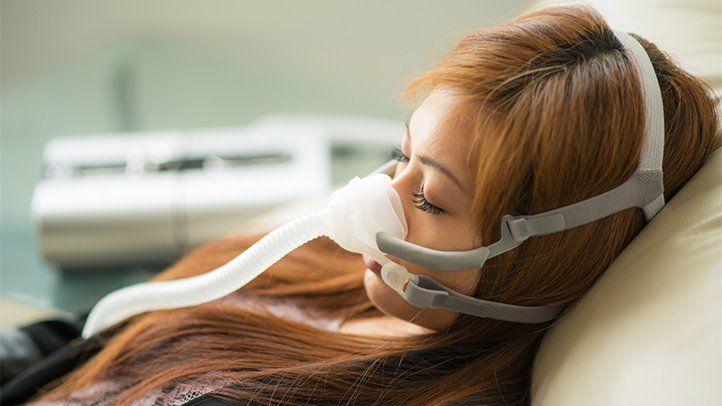
Fortunately, OSA can be treated in several ways. The quality of sleep and control of hypertension may both improve with treatment. Continuous positive airway pressure is the gold standard treatment (CPAP).
The CPAP therapy is using a mask to breathe in pressurized air while sleeping. It helps those who suffer from OSA sleep better by preventing their airway from closing during the night. Treatment with CPAP reduces blood pressure both during the day and at night, notably in individuals with severe OSA, as proven in studies of its effects on hypertensive and OSA patients. Catecholamine suppression is another effect of CPAP.
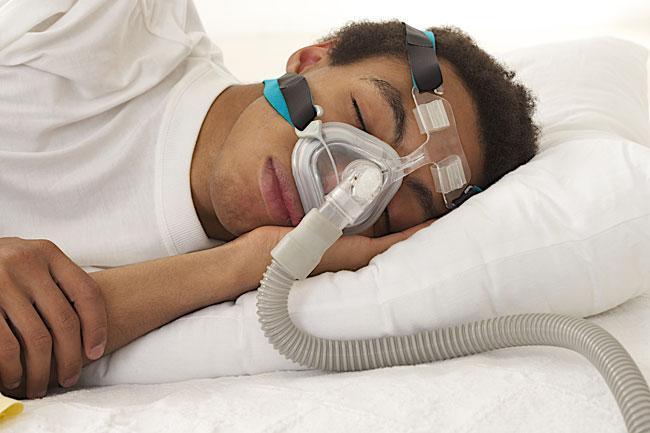
Using a CPAP facemask at night might be uncomfortable for some people. Consistent, appropriate CPAP use is crucial for the efficient management of OSA and hypertension. As an alternative to CPAP, mouthpieces have been developed to keep the airway open while you sleep. There has to be more investigation into whether or not patients with high blood pressure and OSA can benefit from using mouthpieces to reduce their blood pressure. OSA can also be treated by the use of surgical treatments for certain people.
One method of treating OSA that has the added benefit of potentially reducing blood pressure is achieving and maintaining a healthy weight by dietary and lifestyle modifications or surgical intervention.
Should I Talk To My Doctor About Sleep Apnea?
Get checked out by a doctor if you have hypertension and suspect you may possibly have sleep apnea. A proper diagnosis is the first step toward receiving treatment for OSA, which may lead to better sleep and reduced blood pressure. Think about whether any of these symptoms seem familiar:
- Drowsiness during the day.
- Issues paying attention and remembering things.
- Discomfort first thing in the day due to a headache.
- Having a dry tongue upon awakening.
- Mood swings, nervousness, or melancholy.
People with sleep apnea frequently deny that they have the condition. Many cases of obstructive sleep apnea (OSA) are diagnosed after a bed partner has noticed nocturnal symptoms. If you live with other people, you may want to find out if they have seen any of these behaviors from you while you were asleep:
- Very annoying snoring.
- Awaking gasping for air from a choking or suffocating sleep state.
- Having trouble breathing at night.
One should discuss sleep with their doctor if they have any of these symptoms.
Nguồn: https://www.sleepyheadpillowcase.com
Danh mục: Sleep Advisors















