The head of the esophageal and swallowing center at Metro Health Medical Center, Case Western University, Cleveland, OH, is the chair of the division of gastroenterology and hepatology at Case Western.
- How To Design Your Bedroom For A Better Sleep? Update 05/2026
- Signs Your Baby Is Going Through The 8-Month Sleep Regression – Sleep Tips Update 05/2026
- How To Sleep With Noise? Helpful Tips To Remember Update 05/2026
- Best Baby Co-Sleepers – Buyers Guide & Reviews Update 05/2026
- What Is Jet Lag? Symptoms, Causes, Prevent, and Treatment Update 05/2026
Researcher in Clinical Science Senior Investigator Award for Dr. Fass was given out by the IFFGD in 2011. His other research initiatives include those aimed at improving knowledge, diagnosis, and treatment of GERD, functional heartburn, noncardiac chest pain, GERD in individuals who do not respond to PPI medication, and various investigations in patients with gastroparesis. Additionally, studies are being conducted to assess the influence of stroke and the involvement of the brain in esophageal symptoms, as well as a basic science initiative to identify particular markers in patients with Barrett’s esophagus.
Bạn đang xem: How Does GERD Affect My Sleep? Getting a Good Night’s Sleep Update 05/2026
The most frequent condition of the esophagus is GERD, a chronic disorder. GERD-related symptoms are reported by as many as one in five (20 percent) of the adult population in the United States on a weekly basis. Studies have shown that up to 79 percent of GERD patients report overnight symptoms. Many patients with nighttime heartburn said that their symptoms interfered with their sleep, and nearly half (40 percent) noted that their symptoms hindered their ability to work the next day.
“Nighttime reflux is associated with more aggressive symptoms of GERD.”
A bi-directional association between GERD and sleep has been established in the literature. GERD has been demonstrated to disrupt sleep by causing people to wake up in the middle of the night because of their symptoms. More often than not, persons with GERD suffer from sleep fragmentation as a result of frequent, brief wakeups that they can’t seem to recall. As a result of increasing esophageal hypersensitivity and possibly increasing esophageal acid exposure time, sleep loss itself might worsen GERD symptoms.
Erosive esophagitis or inflammation of the esophagus, complications of GERD (such as Barrett’s and cancer of the esophagus), and GERD complications are all associated with nighttime reflux. People who suffer from nighttime reflux are also more likely to experience sensations in their mouths and airways (oropharyngeal, laryngeal, and pulmonary manifestations).
GERD’s extraesophageal symptoms, such as hoarseness, throat-clearing, sore throat, wheezing, and chronic cough, have recently included poor quality of sleep and a variety of sleep disruptions. Also of major concern: Those with midnight heartburn report much lower overall health and well-being compared to those with only daytime heartburn.
When it comes to researching GERD and sleep disorders, the Neuroenteric Clinical Research Group has been working hard for the past decade. The combination of actigraphy (a watch-like device that can tell if a patient is asleep or awake) with their pH test measuring acid exposure matched by time helped us better understand the impact of GERD on sleep. Using both of these methods, we are able to establish a link between the occurrence of gastroesophageal reflux disease symptoms and the time spent sleeping and awake.

We were able to show through a series of research that the time spent in bed just before going to sleep is a sensitive period for gastroesophageal reflux to occur. The amount of esophageal acid exposure increases according to the amount of time spent awake in bed.
People with gastroesophageal reflux disease (GERD) were found to wake up many times during the night, according to our findings. It was shown that only half (50 percent) of the patients woke up because of gastroesophageal reflux (GERD). G.E. reflux-related awakenings were not correlated with symptoms, showing that persons who have GERD may wake up from sleep with considerable reflux yet not experience any symptoms.
After a person wakes up from a deep sleep, the majority of acid reflux incidents occur. Getting up in the morning was found to be connected with a considerable amount of reflux, as we also discovered. Those who suffer from gastroesophageal reflux disease (GERD) are more likely to experience substantial reflux when they get up in the morning. In our trials, deep sleep has been found to be an effective treatment for gastroesophageal reflux disease (GERD).
A key finding of our research was the relevance of limiting the number of times persons with GERD spent awake in bed. Because of this, we just began research in which we evaluated the usefulness of a prescription sleep aid called ramelteon (a melatonin receptor agonist) on symptoms of GERD while sleeping. During a six-week study, patients with GERD got only ramelteon before going to bed; a control group received a placebo. The study found that participants who took ramelteon at sleep for six weeks experienced considerably decreased nocturnal GERD symptoms. A better night’s sleep, as measured by a questionnaire, was found to be a mediating factor.
Taking a nap may increase your risk of gastric reflux disease, according to a recent study we conducted. G.E.R. is more likely to occur in those who take naps because they sleep more shallowly. Taken together, the combination of a nap after eating and gastric reflux disease may be even more severe.
Taking a nap during the day was found to be significantly more frequently connected with symptoms of gastroesophageal reflux disease (GERD) than taking a nap at night.
Our next step is to see if drugs that improve sleep can help persons with GERD who are experiencing symptoms while they sleep. In order to alleviate the symptoms of GERD, we plan to use a combination therapy that includes both an antireflux medication and a sleeping tablet such as a melatonin receptor agonist.
Healthy Sleep
Anyone who suffers from a chronic illness such as functional gastrointestinal (GI) or motility disorders has to prioritize getting enough rest. Your digestive system may be affected by a lack of sleep. The quality of your sleep might also be affected by the symptoms of gastrointestinal diseases. It helps to have a little understanding of sleep science to better appreciate the significance of getting enough shut-eye. It’s also a good idea to learn about ways to make sleeping better.

Different Stages of Sleep
Non-rapid eye movement (NREM, stages 1–4) and rapid eye movement (REM, stage 5) sleep are the two basic states of sleep. Getting a good night’s sleep requires completing each step of the cycle.
- Stage 1: It’s a transitional state between waking and falling asleep. Muscle activity slows down at this point.
- Stage 2: The body temperature decreases, the brain waves slow down, and the respiration and heart rate remain constant in the second stage of sleep.
- Stage 3–4: These stages of sleep are the most restorative. The heartbeat slows, the blood pressure lowers, and muscular action halts as a result of the hypoxia. Tissue repair and energy restoration are both accomplished. This is also the time when the body releases hormones that aid in growth and development.
- Stage 5: Stage 5 is the only stage of REM sleep. Rapid and erratic breathing occurs. Blood pressure and heart rate both rise as a result. As the muscles relax even further, the body and mind are given a boost of energy. Dreams arise during this time. In addition, research shows that REM sleep activates the portion of the brain that is involved in memory and learning.
Effects of Sleep
Your physical, mental, and emotional well-being depend on a good night’s sleep. There are a few benefits to a good night’s sleep:
- Having a clear head
- The ability to respond rapidly
- The process of preserving the past
- Concentrating your efforts on a limited number of projects
- Increasing Your Muscle Size
- Infection-fighting hormones are released during cell and tissue repair.
- the ability to manage the body’s consumption of energy
- Dealing with suffering
Tips for Improving Your Sleep Habits
If you’re having trouble getting a good night’s sleep, here are some simple methods to help. Your doctor should be consulted if you continue to have difficulty sleeping or if you do not feel rested throughout the day despite spending the night in bed.
- Maintain a regular bedtime routine. Establish a regular bedtime and wake-up time (even on weekends).
- Exercise. Make fitness a part of your daily routine.
- Avoid the use of coffee and nicotine. Caffeine’s effects might last up to eight hours before they wear off.
- Alcohol should not be consumed before going to sleep. Having a few drinks before bedtime keeps you awake and alert.
- It’s best to avoid eating or drinking a lot late at night. Both reflux and frequent restroom visits are possible side effects of this condition.
- Reflux can be triggered by taking a nap soon after eating.
- You should avoid snoozing after 3 pm. It’s possible that it’ll make it difficult for you to get to sleep at night.
- Before you go to sleep, take some time to unwind. A portion of your nightly routine should include this.
- Make your bedroom a comfortable place to sleep. Discard anything that can disrupt your sleep, such as televisions, computers, and other sources of bright light or loud noise.
- Keep your eyes closed at night. You should get out of bed if you have been awake for more than 20 minutes to do something soothing till you fall asleep.
What Is GERD?
GERD is a chronic illness characterized by frequent and debilitating heartburn.
Heartburn is a common symptom of reflux disease, which occurs when stomach acid rises into the esophagus and causes burning or churning. Normally, the lower esophageal sphincter (LES) acts as a barrier to prevent this from happening, but if those muscles are weak or relaxed and don’t close all the way, reflux can occur.
In most cases, reflux is minor, rare, and disappears on its own for the vast majority of people.
Xem thêm : How To Cool A Room During Summer? and How the Body Keeps Cool? Update 05/2026
GERD patients, on the other hand, often experience acid reflux at least once a week, and the symptoms are often more severe and painful. Even though it’s typically regarded as something that only affects adults, it can harm youngsters as well.
What Are the Symptoms of GERD?
The most frequent symptom of GERD is heartburn, which causes a burning sensation in the chest, although not all instances of GERD are caused by heartburn.
It is normal for people with gastroesophageal reflux disease to regurgitate a little amount of stomach acid, as well as a few pieces of food.
Coughing and choking can be brought on by stomach acid leaks rising to the mouth and throat. Hoarseness and sore throat are both possible side effects. The term dysphagia refers to a patient’s inability to swallow or the sensation that something is clogging their throat.
Additionally, GERD can induce radiating chest pain that may radiate to other parts of the body such as the neck, jaw, or arms in addition to heartburn. This pain may last anywhere from minutes to hours. People with gastroesophageal reflux disease (GERD) are more likely to wake up in the night because of this sensation.
Why is GERD Worse After Going to Bed?
After going to bed, the symptoms of gastroesophageal reflux disease (GERD) tend to worsen.
- Gravity no longer aids in lowering stomach acid when lying down, making reflux more likely.
- When you sleep, you don’t swallow as much, which reduces the force that drives stomach acid down.
- During deep sleep, saliva production decreases, making it difficult to neutralize stomach acid.
A combination of these factors may make it easier for stomach acid to flow into the esophagus and allow the acid to remain there for longer, increasing the risk of more severe GERD symptoms, including sleep disturbances. Going to bed just after eating or eating items that are known to worsen GERD can exacerbate the situation even worse.
What Are the Health Consequences of GERD?
There are major consequences to long-term acid reflux and GERD. Esophageal inflammation and ulcers, scar tissue that narrows the esophagus, airway spasms, chronic cough, tooth damage, and increased asthma symptoms are just a few of the side effects.
Barrett’s esophagus occurs in roughly 10% to 20% of instances of gastroesophageal reflux disease (GERD). Barrett’s esophagus is the primary risk factor for esophageal cancer, but not everyone with the condition develops the disease.
What Causes GERD?
Other factors have been shown to increase the risk of developing GERD, such as a weak lower esophageal muscle and a family history of the ailment.
These factors increase the likelihood of having gastroesophageal reflux disease. While these risk factors are present in many people, not everyone who has GERD has these risk factors.
- Obesity: People who are overweight or obese are more likely to suffer from gastroesophageal reflux disease (GERD), but the exact reason for this is unknown.
- Smoking Cigarettes: Pressure at the lower esophageal sphincter can be affected by smoking, which may impede stomach acid clearance.
- Drinking Alcohol: Acid indigestion can be exacerbated by the effects of alcohol on the esophageal and stomach emptying processes.
- Using Certain Medications: Many drugs, including anti-asthma, blood pressure, antidepressant, and sedatives, can increase the risk of reflux.
- Hiatal Hernia: This syndrome causes the stomach to rise over the diaphragm, increasing the likelihood of reflux.
- Dietary Choices: Heartburn or reflux can be brought on by a number of different foods and beverages. Chocolate, tomatoes, spicy food, vinegar, citrus, fatty foods, fizzy beverages, coffee, and mint are just a few examples.
- Pregnancy: GERD is common among expecting mothers, although it normally goes away after the baby is born.
How Are GERD and Sleep-Related?
According to the National Sleep Foundation’s 2001 Sleep in America Poll, GERD is a common cause of insomnia. Nearly 60 percent of respondents with frequent heartburn said it interfered with their sleep, and over 30 percent said it hampered their ability to function normally during the daytime, according to a more recent survey.
Heartburn, coughing, and other GERD symptoms that flare up after lying down might make it difficult to get to sleep at night. These signs and symptoms have been linked to poorer sleep quality in GERD patients, according to research conducted in sleep clinics.
GERD and Obstructive Sleep Apnea
Obstructive sleep apnea (OSA), a sleep disease characterized by pauses in breathing while asleep, has been linked to GERD in recent studies. In the medical community, professionals are debating whether GERD causes OSA or GERD causes OSA.
At night, it is likely that GERD causes apneas since it affects the airway and breathing abilities. During the same time, those who suffer from OSA are more likely to experience GERD symptoms since they wake up frequently at night. OSA may cause the esophagus to be more vulnerable to reflux because of a lack of sleep.
GERD and OSA risk can be exacerbated by alcohol, smoking, and obesity, therefore it’s possible that these factors have a role in the observed association.
Even though more research is needed to determine the specific link between GERD and OSA, it is obvious that the two disorders can coexist and cause substantial issues with a person’s sleep, comfort, and general health when they do.
How Can People With GERD Get Better Sleep?
Anxieties and insomnia are common complaints among those suffering from gastroesophageal reflux disease (GERD). Despite the fact that there is no one-size-fits-all cure, there are substantial actions you can take to alleviate heartburn and GERD and obtain a better night’s sleep.

Work With a Doctor
If you have a long history of GERD symptoms and/or frequent sleep or daytime sleepiness, you should visit a doctor. A doctor is an ideal person to analyze the condition, determine the possible cause, conduct appropriate tests, and propose therapy for these complex medical issues.
When treating GERD, a doctor may choose to focus on treating the underlying problem, such as sleep apnea, in order to reduce the number of nocturnal awakenings.
Medical and non-medical ways of treatment are both viable solutions. It is best to consult a doctor about the benefits and disadvantages of these treatments, as they are tailored to each patient’s specific situation.
Lifestyle Changes
Managing GERD often necessitates making alterations to one’s way of life in order to eliminate or minimize the presence of triggers. Reducing one’s intake of hot and acidic foods, keeping a healthy weight, and quitting smoking are just a few examples.
Xem thêm : Can You Overdose On Melatonin? Perfect Information For You! Update 05/2026
Because GERD symptoms often worsen at night, several dietary and lifestyle adjustments are geared toward improving sleep quality for those with GERD.
- Avoid eating late. Reducing the risk of reflux by waiting at least three hours after a meal before going to sleep can help.
- Sleep on your left side. People with gastroesophageal reflux disease (GERD) should sleep on their left side, according to numerous studies. When you sleep on your left side, your esophagus is less likely to be exposed to stomach acid. Reflux is more likely to occur if you sleep on your back.
- Raise the head of the bed: Reflux can be minimized when lying down by raising the head of the bed (not only the pillows under your chin). With an adjustable bed frame and the right mattress, this alteration may be implemented easily.
Medication
In certain cases, lifestyle adjustments alone are not enough to alleviate the symptoms of GERD, and medications may be required.
Antacids, for example, are available over-the-counter and can provide brief relief, but their efficacy is debatable for many people. Acid production in the stomach can be reduced using other medications such as proton pump inhibitors (PPIs) and H2 blockers (H2 antagonists). It’s advisable to check with a doctor before taking any of these medications, whether they’re over-the-counter or on a prescription.
Sometimes, when neither lifestyle changes nor drugs are working to relieve GERD symptoms, a patient’s doctor may recommend surgery.
Improve Sleep Hygiene
In order to sleep better, people with GERD may benefit from examining their sleep hygiene, which encompasses all of the factors that influence their sleep environment and sleep behaviors.
Reduce the number of times you wake up during the night by practicing good sleep hygiene. There are many sleep-related lifestyle adjustments that are also applicable to those with GERD, such as cutting back on caffeine and alcohol use. Other important aspects of good sleep hygiene include maintaining a regular sleep schedule, relaxing before-bedtime rituals, and a peaceful sleeping environment.
How to Improve Your Sleep When You Have GERD
Chronic acid reflux into the esophagus is a symptom of gastroesophageal reflux disease (GERD). This results in annoyance. Acid reflux and heartburn are common, but if you get them more than twice a week, you may have gastroesophageal reflux disease (GERD). It is possible that GERD can cause more serious health issues such as sleep disturbances if it is not treated.
In individuals ages 45 to 64, GERD is a leading cause of disrupted sleep, according to the National Sleep Foundation (NSF). According to an NSF survey, persons in the United States who suffer from nocturnal heartburn are more likely than those who do not to experience the following sleep-related symptoms:
- insomnia
- daytime sleepiness
- restless leg syndrome
- sleep apnea
People with sleep apnea are more likely to suffer from GERD. It is possible to have sleep apnea when your breathing is either shallow or paused during sleep. A few seconds to many minutes may go between these interruptions. This might happen as many as 30 times an hour. These pauses in breathing are followed by a loud snort or choking sound, which is usually followed by a return to normal breathing.
Because it interferes with restful sleep, sleep apnea can leave you feeling groggy and drowsy during the day. It’s more often than not a long-term issue. As a result, it can have a negative impact on day-to-day functioning and make it difficult to focus on routine tasks. The National Sleep Foundation recommends screening for sleep apnea in those with nighttime GERD symptoms.
Coughing and choking are common GERD symptoms, and they seem to get worse while you’re lying down or trying to sleep. This overflow of acid can reach as high as your throat and larynx, which can cause you to feel like you’re coughing or gasping for air. As a result, you may wake up from a deep slumber.
There are several strategies to enhance your sleep if you’re experiencing any of these symptoms. Even if you have GERD, making small changes to your daily routine and behavior can make a big difference in your ability to obtain a good night’s sleep.
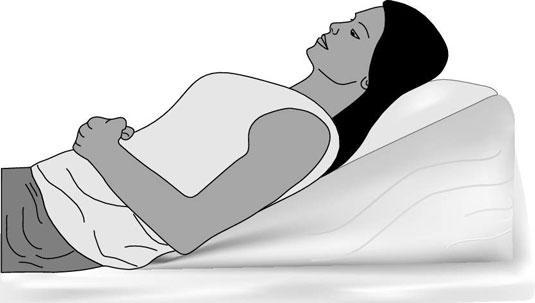
Use a sleep wedge
GERD sufferers may find that using a large wedge-shaped pillow while they sleep helps them sleep better. Because it’s wedge-shaped, the pillow helps keep you partially upright, which in turn helps to reduce acid flow. Other sleeping positions that put pressure on the abdomen and worsen heartburn or reflux symptoms are also restricted.
Maternity shops may have sleep wedges if you can’t find them at a typical bedding store. These businesses frequently stock wedge pillows due to the prevalence of GERD among pregnant women. You can also check out medical supply stores, drugstores, and specialty sleep stores for additional options.

Incline your bed
If you lift your head by tilting your bed’s head forward, you may lessen the likelihood of acid refluxing into your throat while you sleep. Bed risers are recommended by the Cleveland Clinic. The legs of your bed are supported by little, column-like platforms that are inserted under them. They’re frequently employed to free up space for storage. The vast majority of stores selling housewares carry them.
GERD sufferers should not use risers beneath their bed’s footboard; instead, they should place them under the bed’s two top legs (the headboard end). Aim to keep your head higher than your feet at all times. Increasing the height of your bed’s headboard by six inches can be beneficial.
Wait to lie down
GERD symptoms might worsen and interfere with your sleep if you go to bed too soon after eating. The hospital in Cleveland, Ohio, Trusted Source recommends waiting three to four hours after eating before going to sleep. Snacks before going to bed should also be avoided.
Spend some time after supper walking your dog or taking a leisurely stroll through your neighborhood. In the event that a nighttime walk is not feasible, cleaning the dishes or folding clothes can often allow your digestive system time to begin processing your food.
Research According to a study from a reputable source, regular physical activity helps enhance and regulate sleep. Additionally, it aids in weight loss, which in turn lowers the symptoms of GERD. Exercise, on the other hand, naturally raises levels of adrenaline. To put it another way, exercising soon before going to bed can make it more difficult to get to sleep and stay asleep.
Another strategy to reduce reflux is to lose weight. Weight loss reduces intra-abdominal pressure, which lowers the risk of reflux.
Eat smaller, more frequent meals and stay away from foods and drinks that aggravate your symptoms, like large, heavy meals. The following meals and beverages should be avoided, according to the Mayo Clinic:
- fried foods
- tomatoes
- alcohol
- coffee
- chocolate
- garlic
What’s the takeaway?
However, GERD symptoms can have a substantial impact on the quality of your sleep, but there are measures you can do to lessen those symptoms. In the event that you’re unable to sleep due to GERD, lifestyle changes such as decreasing weight may be necessary.
Some persons with gastroesophageal reflux disease (GERD) require medicinal treatment in addition to lifestyle adjustments. It’s your doctor’s job to help you design a treatment plan that’s tailored to your needs.
Nguồn: https://www.sleepyheadpillowcase.com
Danh mục: Sleep Advisors















